At TheHealthBoard, we're committed to delivering accurate, trustworthy information. Our expert-authored content is rigorously fact-checked and sourced from credible authorities. Discover how we uphold the highest standards in providing you with reliable knowledge.
What is a Lower Endoscopy?
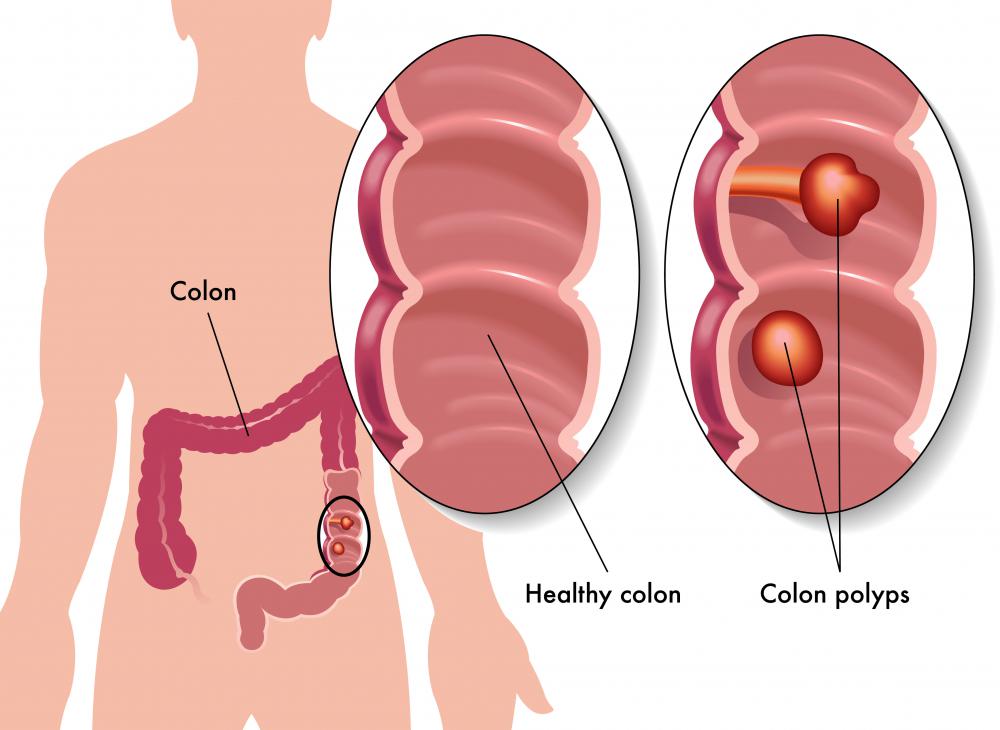
A lower endoscopy is an examination of the lower gastrointestinal (GI) tract with an endoscopic camera inserted through the anus. The rectum, colon, and sigmoid colon are carefully inspected in a procedure that combines a colonoscopy and a sigmoidoscopy. Lower GI endoscopy may be used to identify inflammation, remove polyps, biopsy tissue samples, or diagnose cancer.
Some prescription and over-the-counter medications should not be taken before the lower endoscopy. To reduce the risk of excessive bleeding from an accidental nick in the colon during the exam, non-steroidal anti-inflammatory drugs (NSAIDs) should be discontinued a week before the appointment. People who take blood thinners, such as heparin, may need to be medically supervised during the temporary suspension of anti-coagulant medications.

The colon must be completely empty before the lower endoscopy. A liquid diet may be advised one to two days before the examination. Most people are asked to stop eating a minimum of twelve hours before the lower endoscopy appointment, due in part to the risk of side effects from the anesthesia given during the procedure, and also the need for an empty digestive tract.

To ensure the colon is cleansed of all fecal matter, an enema is usually required the night before and the morning of the lower endoscopy procedure. The addition of fluid to the rectum and colon increases the peristaltic movements of the intestines, flushing out the contents quickly. A laxative may be added to the regimen to encourage the rapid expulsion of fecal contents before the endoscopic exam.

Before the lower endoscopy, anesthesia and a sedative may be given to relax the patient during the exam and to eliminate any uncomfortable sensations that may occur as the exam progresses. These two medications are usually administered through an intravenous (IV) line. Due to the sedative and anesthesia, the patient’s vital signs will be carefully monitored throughout the procedure.
During the lower endoscopy, the patient will be lying on his left side. A long thin tube with a fiber optic lens is gently inserted into the anus. Short puffs of air may be sent through the tube into the colon to enable the doctor to easily visualize the interior lining. If any suspicious looking tissue is seen, a biopsy may be taken through the endoscopic instrument. A polypectomy can be done immediately to remove any polyps seen during the examination.
After the exam is completed, the patient will still be affected by the anesthetic and sedative used for the procedure. Most people are advised not to make any financial or legal decisions within 24 hours of the exam. The patient will not be able to safely drive after the appointment, and will need to be driven home. Results of any biopsy taken should be available within seven days of the exam.
AS FEATURED ON:
AS FEATURED ON:












Discuss this Article
Post your comments